Without effective antibiotics to prevent and treat bacterial infections, the achievements of modern medicine will be jeopardized. It will be difficult or even impossible to treat bacterial infections and recovery will be prolonged, leading to increased morbidity and mortality for severely ill patients. Chemotherapy for cancer, intensive care, care of preterm babies and routine surgical procedures might all be considered too dangerous in the future, due to the high risk of difficult-to-treat infections.

Cross-border cooperation is needed to fight antibiotic resistance. Sweden has been instrumental in highlighting and emphasizing the problem, both within the EU and globally. We made it a high priority issue in 2009 when we held the Presidency of the Council of the European Union.

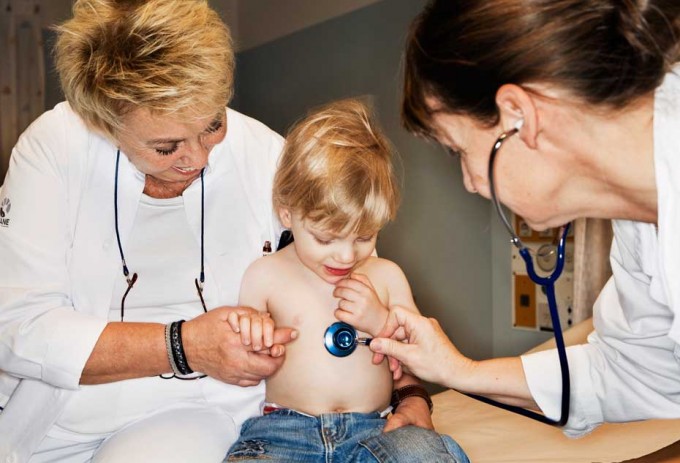
A quick and simple yet accurate white blood cell test at the point of care can help doctors decide whether to use antibiotics or not.
Our commitment has also resulted in the creation of ReAct, one of the first international networks working to combat the growth in antibiotic resistance. ReAct acts as a forum for ideas, debate and collaboration between diverse stakeholders, driven by a vision of a world free from fear of untreatable infections.
Swedish experience has acted as a driving force behind the work on a global plan drawn up by WHO on the ways in which the 194 member states should work to arrest this trend. The overall goal of the plan is to ensure that we secure the ability to treat and prevent infectious diseases using effective and safe medications. And to ensure that antibiotics are used responsibly and made available to everyone who needs them.
The plan has five strategic areas:
- Improve awareness and understanding of antimicrobial resistance
- Strengthen knowledge through surveillance and research
- Reduce the incidence of infection
- Optimize the use of antimicrobial agents
- Develop the economic case for sustainable investment that takes account of the needs of all countries, and increase investment in new medicines, diagnostic tools, vaccines and other interventions.

Infection control at the earliest possible stage, combined with hygiene routines and the right equipment for effective cleaning, disinfection and sterilization, are essential measures to reduce the risk of spreading infections in healthcare environments.
The problem of antibiotic resistance is caused by decades of antibiotic overuse. It is estimated that more than half of all antimicrobials are inappropriately prescribed or dispensed. Sweden is an exception, with one of the lowest antibiotic consumption levels in the world, partly thanks to close control on availability and doctors who know the dangers of over-treatment.
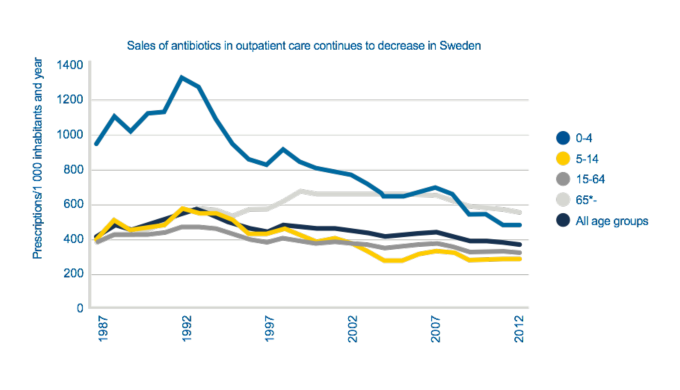
During the past two decades, antibiotic use in Sweden has been reduced by 50% in children under the age of four. This progress has been made without producing any measurable negative outcomes.
The most important reason to Sweden’s positive development over the last decades is a comprehensive strategy to handle the challenge of antibiotic resistance. This strategy has three main pillars:
- We have an open doctor and patient dialogue that promotes a rational use of antibiotics.
- We have invested in technology to monitor the use of antibiotics in our healthcare system.
- We allocate resources to governmental authorities to work with preventive measures.
We have an open doctor and patient dialogue that promotes a rational use of antibiotics.
The clear link between antibiotic resistance and consumption made Sweden draw up national treatment recommendations on how and when to use antibiotics. Sweden regulates sales of medicines and patients can only obtain antibiotics with a prescription issued by a licensed practitioner. Sweden’s pharmacies have been producing statistics on antibiotic sales since the 1970s, providing us with valuable knowledge of changes in prescription trends.
The Public Health Agency of Sweden receives daily updates on these figures, enabling it to draw up treatment recommendations with which the medical sector must comply. Also, Sweden’s advanced national system for electronic prescriptions ensure security and consistency throughout the pharmaceutical supply system.
Sweden was also an early adopter of a strategic programme to combat antibiotic resistance. A national action plan was published in 2000 and acted as an important starting point for Sweden’s ongoing coordinated work to counter antibiotic resistance and healthcare-associated infections. The plan stresses the importance of a cross-sectorial approach.

The most basic of the measures taken to prevent the spread of infection is the consistent application of hygiene routines and appropriate clothing in their work by all categories of medical personnel.
The design of the hospital itself is another important component in preventing healthcare-associated infections and the spread of resistant bacteria. Effective logistics including a safe flow of sterile goods, innovative waste management solutions and a policy of offering single rooms to patients are all important infection control measures.

Together with ASSA, White Architects designed the “ASSA Hygienic Handle” to limit the spread of bacteria.
Good and thoughtful design also characterizes the details at the New Karolinska University Hospital, one of the world’s most modern and sustainable university hospitals which will treat the most seriously ill or injured patients in Stockholm county. Together with ASSA, White Architects designed the “ASSA Hygienic Handle” to limit the spread of bacteria. The handle is ergonomically designed and meets the stringent requirements of modern hospital environments.
The New Karolinska University Hospital will admit its first patient in 2016. The design of the buildings and facilities prioritizes the best of interests of patients. All patient rooms will be single which gives a higher degree of personal integrity and privacy for patients and allows medical staff to work in teams at the patient’s bedside. Also, it contributes to reducing disease transmissions and nosocomial infections.
Sweden’s strategic and focused work to combat antibiotic resistance and prevent healthcare-associated infections has been globally acknowledged – which we naturally are very proud of – but the work is far from over. The challenge posed by multi-resistant bacteria is something all countries must address and combat collectively as bacteria know no borders.
Photo credit: Getinge Group, HemoCue, Mölnlycke Health Care, Sofia Sabel / imagebank.sweden.se